Data Visualizations
The numbers behind the findings
FY2026 CMS dataset. Select a research question to view the analysis.
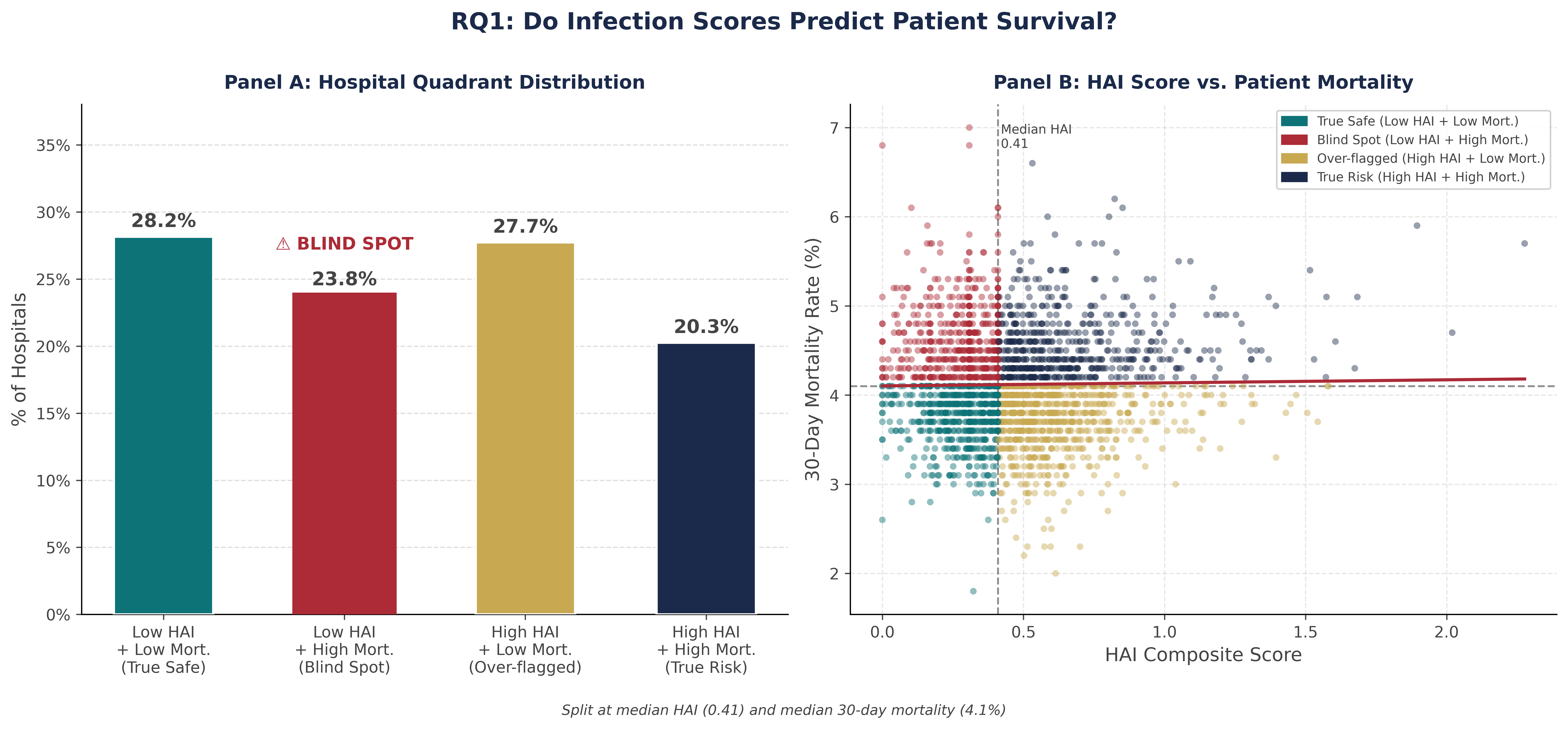
Left: 550 hospitals (19.4%) fall in the blind-spot zone - low HAI composite but above-median mortality. The HAC program detects only 9.8% of them. | Right: Scatter of HAI composite vs 30-day mortality. ■ Blind-spot hospitals ■ All others. Near-zero correlation (r = 0.015) means HAI compliance tells us almost nothing about whether patients survive.
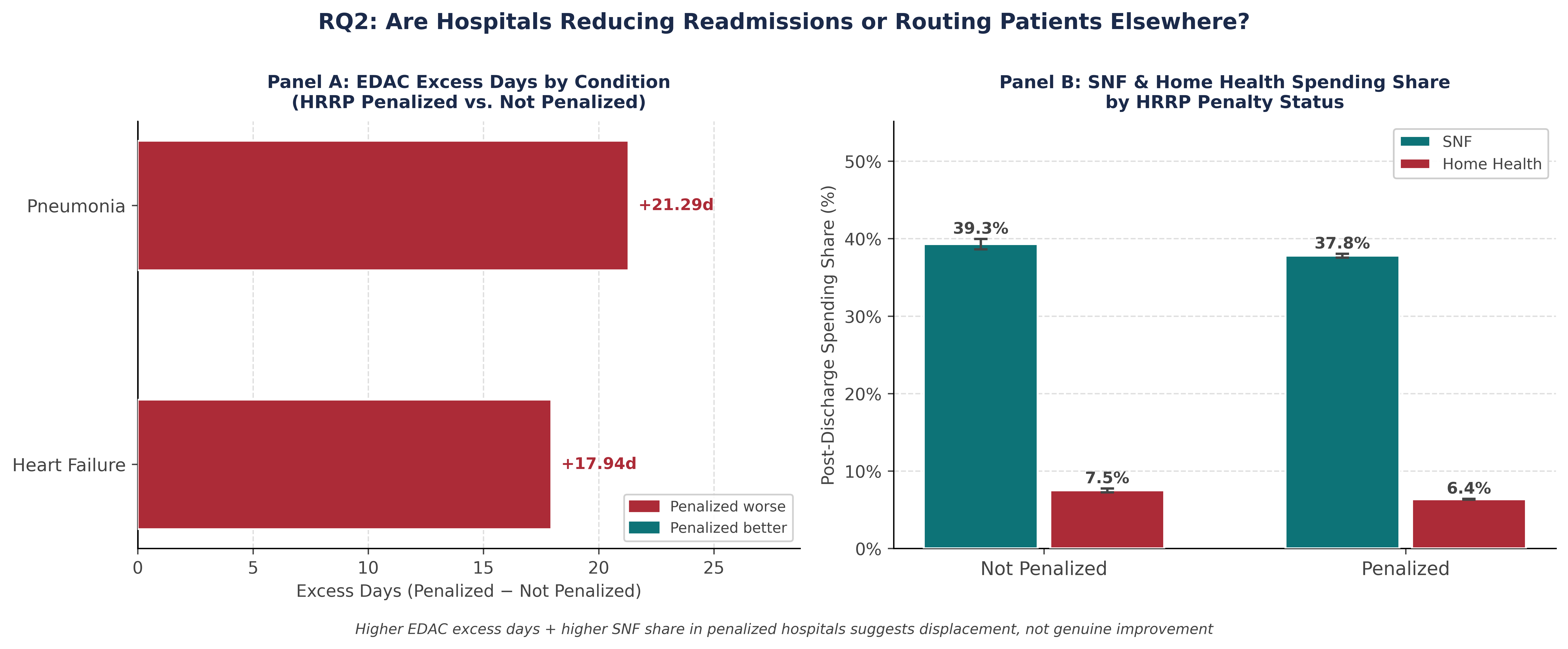
Left: HRRP-penalized hospitals show dramatically higher excess days in acute care (EDAC) post-discharge - +17.9 days for heart failure, +21.3 days for pneumonia. Only 22–24% of this gap is explained by pre-existing quality differences. | Right: Non-penalized hospitals route more spending through SNFs (39.0% vs 38.0%) and home health (7.0% vs 6.0%) - consistent with readmission displacement via post-acute routing.
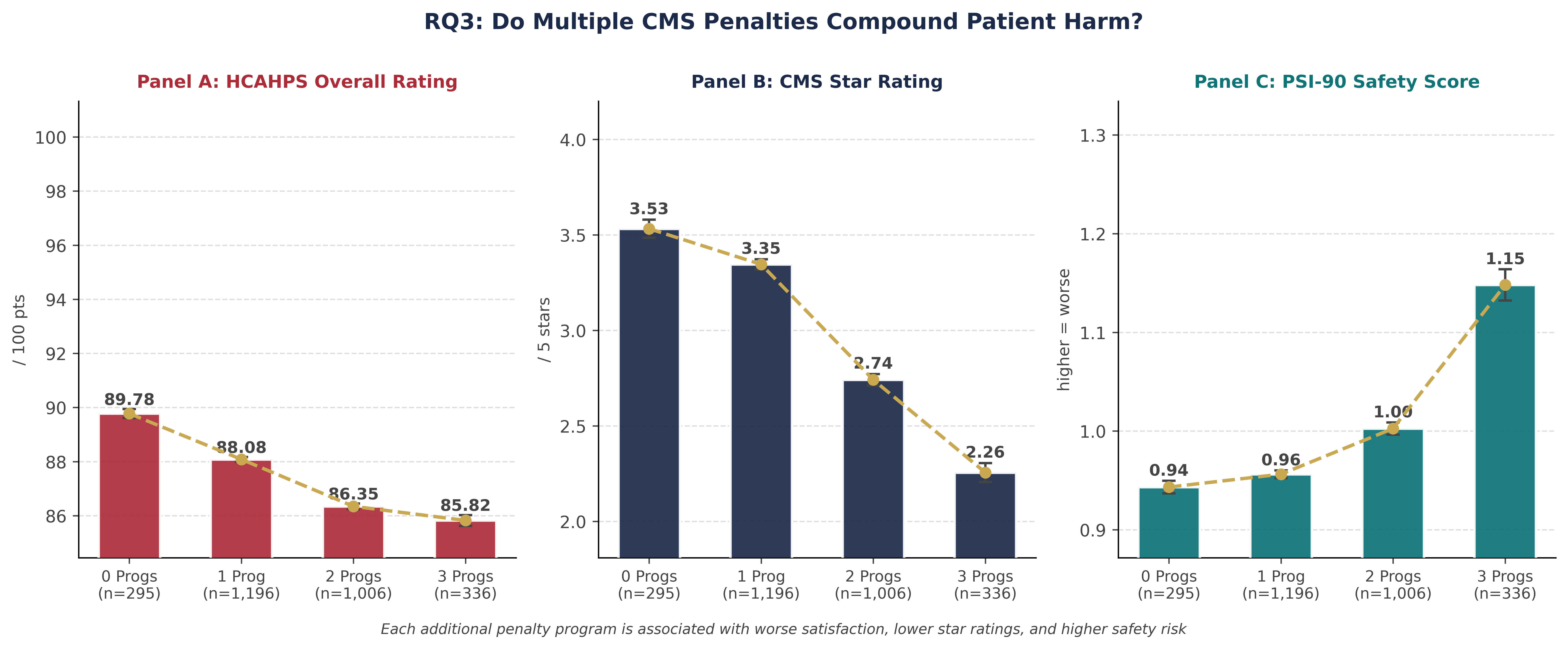
Left: HCAHPS overall rating drops from 89.776 (0 penalties) to 85.824 (3 penalties) - a 3.95-point gap (p < 0.001). | Center: CMS star rating falls from 3.532★ to 2.256★. | Right: PSI-90 composite rises from 0.943 → 1.148 - values above 1.0 indicate worse-than-expected patient safety events. Every additional concurrent penalty is independently associated with worse outcomes across all three measures.